
Cases description of acute thyroid swelling following fine-needle aspiration biopsy: potential hypersensitivity reaction
Introduction
Thyroid nodules are highly prevalent, affecting up to 50–67% of the general population. Among these, approximately 5% are malignant, with papillary thyroid cancer being the most common type. Globally, thyroid cancer incidence rates are higher in women and exhibit significant regional variations, particularly in Eastern Asia and Northern America (1,2).
Fine-needle aspiration (FNA) cytology is a widely used and highly accurate diagnostic tool for evaluating thyroid nodules. Although generally safe and effective, FNA is associated with common minor complications such as local pain, discomfort, and minor hematoma (3-5). Severe complications, including extensive hematoma, infection, or tumor dissemination, are exceedingly rare (6). Of particular clinical interest is a distinct yet poorly understood complication: acute thyroid swelling. First documented in 1982 (3), this phenomenon is characterized by sudden, marked thyroid enlargement following FNA, accompanied by a unique ultrasonographic “cracked” hypoechoic pattern within the gland. Although symptoms commonly resolve spontaneously within 12 hours, sporadic cases may progress to critical complications such as airway obstruction (7). The pathophysiology of acute thyroid swelling remains controversial, with existing speculations about its mechanism lacking robust pathological or experimental evidence. In this study, we present a series of seven cases in which patients experienced acute thyroid swelling following FNA. By retrospectively analyzing these cases and integrating a comprehensive literature review, we aimed to: (I) delineate the clinical and imaging hallmarks of this complication; and (II) evaluate histopathological evidence supporting an allergic mechanism. By synthesizing clinical observations with mechanistic insights, we aimed to promote early recognition of this rare complication and inform future investigations into its underlying biology.
Case presentation
This study was approved by the Ethics Committee of the China-Japan Friendship Hospital (No. 2019-103-K71). All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Declaration of Helsinki and its subsequent amendments. Written informed consent was provided by the patients for publication of this article and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Case 1
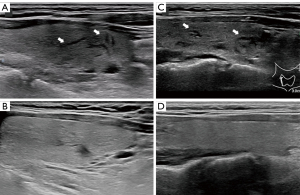
A 34-year-old woman was referred to the hospital due to a high-risk nodule (6 mm × 6 mm × 5 mm) in her right thyroid lobe (Figure 1A,1B). Her thyroid function was normal. Ultrasound (US)-guided FNA with a 23-guage needle was performed on the nodule. No evidence of bleeding or edema was observed at the FNA site, and no hematoma or other abnormalities were found in ultrasonic examination an hour later. No anesthesia was used. The patient had no known allergies or use of specific medication.
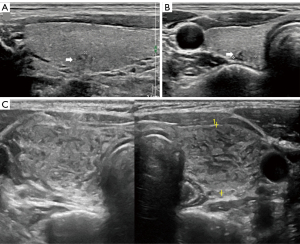
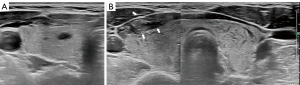
About 2 hours after FNA, the patient returned with complaints of neck swelling and mild pain. US showed diffuse swelling in both thyroid lobes with fine hypoechoic “cracks” (Figure 1C). The thyroid volume had increased approximately 2-fold compared with pre-FNA (Figure 2A,2B), with no blood flow observed in the “cracks” on color Doppler US.
Even after local compression, the thyroid swelling did not significantly change, and over 5 hours, the volume progressively increased to 3- to 4-fold (Figure 2C). Due to the patient’s progressive dyspnea and considering the suspiciously malignant nodule in the right lobe of the thyroid, after thorough communication with the surgeon and the patient, surgery was performed. The rapid intraoperative pathology confirmed that the nodule in the right lobe was papillary thyroid carcinoma, and subsequently, a right thyroid lobectomy was carried out.
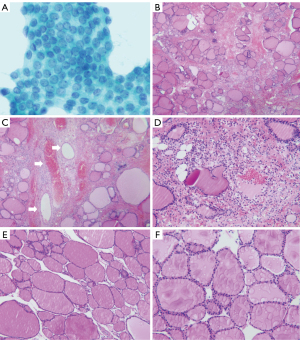
After surgery, the patient’s neck swelling and other complaints subsided (Figure 2D), and she was discharged. Pathological examination revealed papillary carcinoma in the right lobe nodule, with an “island” arrangement of thyroid follicular cells, increased inter-island gaps containing leukocytes, erythrocytes, and fibrous exudates, and observed vascular dilatations within the gland (Figure 3).
Subsequent US performed 7 months later showed no sign of swelling or hematoma, with no change in the left lobe.
Cases 2–7
Following case 1, our research team conducted a total of 3,988 FNA examinations on thyroid nodules between January 2023 and January 2024. Of these, 6 cases experienced acute thyroid swelling after FNA (Table 1). All FNAs were performed with 23-gauge needles without anesthetics. No patient had any history of allergies.
Table 1
| Case No. | Age (years) | Sex | Nodule characteristics (mm) | Start of swelling | Duration | Clinical manifestations | Volume of the thyroid gland (approximately) | Cytological diagnosis | Treatment | Other findings |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 34 | F | 6×6×5 (right lobe) | 2 h after FNA | 12 h | Diffuse neck swelling and tenderness | 3- to 4-fold | Papillary carcinoma | Endotracheal intubation, right-sided thyroidectomy | No |
| 2 | 25 | F | 28×20×16 (left lobe) | 3 h after FNA | 8 h | Diffuse neck swelling and pain | 2-fold | Papillary carcinoma | No | No |
| 3 | 38 | M | 6×8×7 (right lobe); 6×5×6 (left lobe) | During FNA | 30 min | Asymptomatic | No significant changes | Papillary carcinoma | No | No |
| 4 | 51 | M | 18×16×12 (left lobe) | Immediately after FNA | 1 h | Diffuse neck swelling | No significant changes | Follicular neoplasm | Dexamethasone, 5 mg, iv | Abnormal sensation |
| 5 | 46 | F | 5×4×3 (right lobe); 8×6×5 (left lobe) | During FNA | 1 h | Diffuse neck swelling and pain | 1.5-fold | Unsatisfactory | No | Localized hematoma |
| 6 | 33 | F | 4×4×4 (right lobe) | During FNA | 30min | Asymptomatic | No significant changes | Unsatisfactory | No | No |
| 7 | 66 | F | 5×6×4 (left lobe); 4×5×4 (right lobe) | During FNA | 2h | Diffuse neck swelling and pain | 1.5-fold | Benign (left lobe); follicular neoplasm (right lobe) | Dexamethasone, 5 mg, iv | No |
F, female; FNA, fine-needle aspiration; h, hour; iv, intravenous; M, male; mg, milligram; mm, millimeter; min, minute.
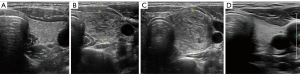
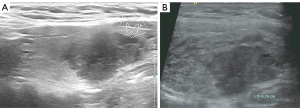
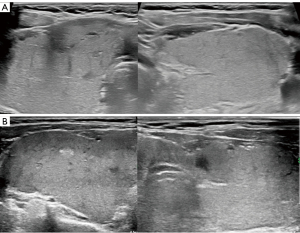
The US pattern in our 6 cases showed a patchy and heterogeneous appearance, with scattered hypoechoic “cracks” and no blood flow signal using Doppler US. Of the 6 cases, 5 showed disappearance of subjective complaints and improvement of thyroid swelling within 2 hours (cases 3–7). Acute thyroid swelling occurred during or immediately after FNA in these 5 cases (cases 3–7) with symptoms appearing 3 hours after FNA in 1 case (case 2) (Figure 4). Two cases were asymptomatic, with abnormalities detected only by US (cases 3 and 6) (Figure 5). All cases experienced thyroid swelling for less than 12 hours. There was 1 patient who developed a localized hematoma after puncture (case 5) (Figure 6) and 2 patients (cases 4 and 7) (Figure 7) received dexamethasone (5 mg, intravenous). The FNA results were papillary carcinoma in cases 1–3, follicular neoplasm in cases 4 and 7, and benign in case 7.
Discussion
Acute thyroid swelling following FNA is a relatively rare complication. Previous studies have reported the prevalence of acute thyroid swelling to be 0.46% (5), 0.15% (8), and 0.13% (9). According to data from the English literature, about 38 cases have been recorded (3,5,7-20). In our research conducted between January 2023 and January 2024, out of 3,988 FNA examinations on thyroid nodules, 6 cases experienced acute thyroid swelling after FNA.
Although acute thyroid swelling following FNA is rare, it is speculated that it may be under-diagnosed and under-reported (21). Nakatake et al. (14) reported 3 cases with this complication in just 6 weeks and Zheng et al. (5) reported an incidence rate of 0.46% in their institute. Our experience of 6 cases during 1 year suggests that this complication may be more common than previously thought. The cases with asymptomatic or only low echo “crack” changes on US are easily overlooked.
Patients with acute thyroid swelling complain of diffuse neck swelling and tenderness, dyspnea, or only mild pain, without airway obstruction or hemorrhage. In our institute, 1 case was endotracheally intubated because of progressive airway obstruction. In addition, Kousaka et al. (7) reported a patient who required endotracheal intubation due to acute thyroid swelling and airway obstruction following FNA. A computed tomography (CT) scan revealed swelling not only of the thyroid but also retropharyngeal space. Laryngeal fiberscopy revealed protrusion of the posterior pharyngeal wall, and edematous changes in the mucosa of the pharynx and epiglottis. The swelling of the thyroid and surrounding tissues rapidly decreased the day after intubation.
A review of previous cases revealed that acute thyroid swelling is not exclusive to FNA. A case of acute thyroid swelling was reported after subclavian vein catheterization (12), and the authors highly suspected that the acute swelling might be related to the puncture of the thyroid. Shi (16) reported the case of a 56-year-old man with diffuse thyroid swelling after thrombolysis with recombinant tissue plasminogen activator (rt-PA) for whom the US findings were similar. After several hours, the pain and swelling completely disappeared. The second US showed that the thyroid volume and appearance were completely restored the next day.
US findings in cases of acute thyroid swelling typically show a patchy and heterogeneous appearance, with hypoechoic “cracks” diffusely scattered throughout the thyroid and no detectable blood flow signals on Doppler US (3,5,7-22). Intrathyroidal hemorrhage was initially suspected in some cases but was ruled out due to the hyperacute swelling and rapid reversibility of the condition. Parenchymal hemorrhage or hematoma typically requires several days to weeks for resolution (16).
Acute thyroid swelling typically occurs within 2 hours after FNA, is self-limiting, and usually resolves within 24 hours. Zheng et al. (5) also reported 4 cases of delayed thyroid swelling occurring 7 hours to 2 days after a successful FNA of a thyroid nodule and subsiding within another 7 hours to 3 days. Dexamethasone, hydrocortisone, and H1-antihistamines were used for anti-inflammatory and anti-allergic treatment in some cases (7,9,17,18,20). Given the small sample size, it is not clear whether steroid administration significantly alters the natural course or duration of acute thyroid swelling (15).
The mechanism of acute thyroid swelling after FNA is unclear. Van den Bruel et al. (11) reported a case of acute thyroid swelling in a patient with medullary thyroid carcinoma, which may be associated with the local release of calcitonin gene-related peptide (CGRP). However, CGRP may not be accountable for most of the reported cases with diagnoses other than medullary thyroid cancer. We speculate that acute thyroid swelling may be a hypersensitivity reaction. When the needle comes into contact with the patient’s skin (external physical stimulus) or the drugs in their body (internal chemical stimulus), mast cells are activated. Inflammatory mediators such as histamine are released, causing changes in vascular permeability, and eventually leading to diffuse swelling of the thyroid gland. When the stimulus is eliminated, the patient recovers spontaneously and the substance is gradually cleared away by the body (17). Pain and swelling of the neck were the main symptoms in our reported cases. Ultrasonography showed mild or significant enlargement of the thyroid volume, and “cracked” low echoes were observed. Some patients had no obvious symptoms, and US showed no significant enlargement of the thyroid volume, or only cracked changes within the gland. In most cases, no treatment was required, and it usually took only 1 hour for the thyroid to return to normal size and related symptoms to disappear. In case 1, the patient had increased pain after FNA, and due to increased airway obstruction, the patient received endotracheal intubation treatment. Combined with the high-risk nodules on the right side, the patient finally chose surgical resection of the right lobe. It is noteworthy that previously unobserved histological features were identified in our images: (I) the thyroid state exhibited an “island” arrangement, with significantly enlarged gaps between these “islands”; (II) the gaps contained a substantial number of leukocytes, erythrocytes, and fibrous exudates; (III) vascular dilatations were observed within the gland. Consequently, we postulate that this phenomenon may be attributed to an allergic reaction induced by FNA or medication. This could explain the “cracking” low echoes on the US images.
This study evaluates the presence of thyroid swelling following FNA biopsy, demonstrating, in a series of 7 cases, the occurrence of this phenomenon. In one of the cases, a more detailed assessment was possible due to the availability of additional histopathological analysis. We present, for the first time, pathological evidence suggesting that acute thyroid swelling may be mediated by hypersensitivity reaction. Furthermore, we propose that this phenomenon is likely underrecognized as opposed to rare. However, this study has several limitations, including the small sample size and retrospective design. Continued data collection with an expanded sample size and a prospective approach, including histopathological analysis, may help to identify other relevant histopathological and ultrasonographic determinants, contributing to a better understanding of the process and its potential implications for clinical management.
In summary, acute thyroid swelling is a self-limiting complication of FNA characterized by symmetrical neck swelling and pain, and US findings of a thyroid volume increase of 1- to 5-fold with “cracked” hypoechoic areas. This complication resolves on its own within 24 hours. We speculate that this is an allergic reaction, so it is important to understand such complications to avoid unnecessary intervention.
Acknowledgments
None.
Footnote
Funding: The present study was supported by
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://qims.amegroups.com/article/view/10.21037/qims-24-1333/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. This study was approved by the Ethics Committee of the China-Japan Friendship Hospital (No. 2019-103-K71). All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Declaration of Helsinki and its subsequent amendments. Written informed consent was provided by the patients for publication of this article and accompanying images. A copy of the written consent is available for review by the editorial office of this journal.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Kobaly K, Kim CS, Mandel SJ. Contemporary Management of Thyroid Nodules. Annu Rev Med 2022;73:517-28. [Crossref] [PubMed]
- Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, Jemal A. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 2024;74:229-63. [Crossref] [PubMed]
- Haas SN. Acute thyroid swelling after needle biopsy of the thyroid. N Engl J Med 1982;307:1349. [Crossref] [PubMed]
- Wong R, Farrell SG, Grossmann M. Thyroid nodules: diagnosis and management. Med J Aust 2018;209:92-8. [Crossref] [PubMed]
- Zheng BW, Wu T, Xu SC, Yin TH, Tan L, Lian YF, Ren J. Acute transient swelling of the thyroid following fine-needle aspiration: A case series. J Clin Ultrasound 2022;50:236-42. [Crossref] [PubMed]
- Polyzos SA, Anastasilakis AD. Clinical complications following thyroid fine-needle biopsy: a systematic review. Clin Endocrinol (Oxf) 2009;71:157-65. [Crossref] [PubMed]
- Kousaka J, Imai T, Saito M, Banno H, Ito Y, Ido M, Goto M, Ando T, Mouri Y, Fujii K, Nakano S. Airway obstruction requiring tracheal intubation after fine-needle aspiration of the thyroid gland: a case report. BMC Surg 2022;22:28. [Crossref] [PubMed]
- Yamada K, Toda K, Ebina A, Motoi N, Sugitani I. Ultrasonographic and non-enhanced CT features of acute transient thyroid swelling following fine-needle aspiration biopsy: report of four cases. J Med Ultrason (2001) 2015;42:417-25. [Crossref] [PubMed]
- Uchida T, Himuro M, Komiya K, Goto H, Takeno K, Honda A, Sato J, Kawano Y, Suzuki R, Watada H. Evanescent Hyperechoic Changes After Fine-Needle Aspiration Biopsy of the Thyroid in a Series With a Low Overall Prevalence of Complications. J Ultrasound Med 2016;35:599-604. [Crossref] [PubMed]
- Dal Fabbro S, Barbazza R, Fabris C, Perelli R. Acute thyroid swelling after fine needle aspiration biopsy. J Endocrinol Invest 1987;10:105. [Crossref] [PubMed]
- Van den Bruel A, Roelandt P, Drijkoningen M, Hudders JP, Decallonne B, Bouillon R. A thyroid thriller: acute transient and symmetric goiter after fine-needle aspiration of a solitary thyroid nodule. Thyroid 2008;18:81-4. [Crossref] [PubMed]
- Bouwman RA, Meijerink MR, Beishuizen A. Acute transient thyroid swelling after catheterization of the subclavian vein. Crit Care 2009;13:419. [Crossref] [PubMed]
- Norrenberg S, Rorive S, Laskar P, Catteau X, Delpierre I, Avni FE, Salmon I. Acute transient thyroid swelling after fine-needle aspiration biopsy: rare complication of unknown origin. Clin Endocrinol (Oxf) 2011;75:568-70. [Crossref] [PubMed]
- Nakatake N, Fukata S, Tajiri J. Acute transient thyroid swelling after fine-needle aspiration biopsy: three cases during only 6 weeks - a rare complication? Clin Endocrinol (Oxf) 2012;77:152-4. [Crossref] [PubMed]
- Tang WK, Bhatia KSS, Pang ASW, Ahuja A. Acute diffuse thyroid swelling: A rare complication of fine-needle aspiration. J Clin Ultrasound 2017;45:426-9. [Crossref] [PubMed]
- Shi L, Yan C, Xu W, Huang P. Acute diffuse and transient thyroid swelling after intravenous thrombolysis for acute ischemic stroke: A case report. Medicine (Baltimore) 2018;97:e12149. [Crossref] [PubMed]
- Zeng W, Lu J, Yan Z, Liu Y, Deng W, Zhou Y, Xu W, Wang Y, Xu J, Miao Y. Acute transient thyroid swelling after fine-needle aspiration biopsy: A case report of a rare complication and a literature review. Diagn Cytopathol 2022;50:E193-7. [Crossref] [PubMed]
- Imaoka K, Nishihara M, Nambu J, Yamaguchi M, Kawasaki Y, Sugino K. Acute diffuse thyroid swelling after fine-needle aspiration: A case report and review of the literature. J Clin Ultrasound 2021;49:720-3. [Crossref] [PubMed]
- Zhu T, Yang Y, Ju H, Huang Y. Acute thyroid swelling after fine needle aspiration-a case report of a rare complication and a systematic review. BMC Surg 2021;21:175. [Crossref] [PubMed]
- Kim YK, Goak IS, Kim YJ, Jin HY, Lee KA. A rare case of acute transient thyroid swelling without hematoma after fine needle aspiration. Korean J Intern Med 2022;37:693-4. [Crossref] [PubMed]
- Polyzos SA, Anastasilakis AD, Arsos G. Acute transient thyroid swelling following needle biopsy: an update. Hormones (Athens) 2012;11:147-50. [Crossref] [PubMed]
- Sun PF, Lang L, Shi W, Guo J. Acute transient thyroid swelling after core-needle biopsy. J Clin Ultrasound 2019;47:219. [Crossref] [PubMed]


